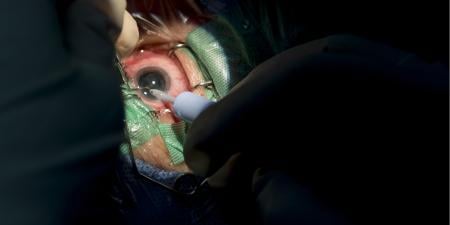
The successful rehabilitation of an individual who has lost an eye requires the attention of several eye care specialists: ophthalmologists, optometrists, opticians—and ocularists. Ocularists are eye professionals whose work is to restore the appearance of an eye lost to trauma, disease, or congenital malformation. Although most eye loss is due to disease, accidents also cause a significant number; of course, only after all vision-saving procedures are exhausted is eye removal considered. Patients are generally referred by the surgeon who operated on the affected eye (often an oculoplastic ophthalmologist) and can tell them what to expect from the ocularist’s work. Those who self-refer must retain realistic expectations for the outcome of their appearance.
This unusual blend of art in medicine is an enterprise all its own. While the ocularist’s work has long been considered an art form, the eye-maker’s role in health care has rarely been clearly-defined. An artificial eye-maker creates custom ocular prostheses or prosthetic eyes, but what we give patients can be much more: improved self-image and the confidence necessary for patients to return to independent, productive living.
Ocular Implants
While evisceration, enucleation, and exenteration all entail the removal of eye tissue, enucleation, the removal of the eyeball from the orbit, remains the most common. Evisceration and enucleation are generally followed by insertion of an ocular implant. To be effective, the implant must reasonably reproduce the volume, position, and motility of the natural eye; it must retain a covering suitable for lubrication and it must neither migrate nor extrude.
The size, material, and placement of the implant depend on the surgeon’s work and the patient’s needs. Generally, a smaller implant is used when it is placed within the eyeball or its fascial capsule (Tenon’s capsule) or when it will be wrapped in another material. To increase covering tissue thickness, the implant is often placed behind the posterior Tenon’s capsule (see figure 1).
Figure 1. Illustration Depicts a Left Post-evisceration Eye Socket in Parasagittal Section.
Caption
The implant replacing the volume of the eye is placed inside the sclera. In front of the repositioned conjunctiva, the custom-made prosthesis is placed under the eyelids.
Proper sizing of the implant is crucial: too small an implant will cause possible migration, exophthalmos, or a deep sulcus. If too large an implant is used, pressure on the front of the implant may increase the risk of wound dehiscence, erosion, or implant exposure and infection. It is ideal for the ocular implant to provide 65-70 percent of the volume of the (lost) eye with the remaining volume taken up by the ocular prosthesis.
In evisceration, the sclera remains, while in enucleation, the extraocular eye muscles are either attached to the implant or cross-sutured and the anterior tissues (Tenon’s and conjunctiva) are closed without tension. Two of the more difficult challenges for ophthalmologists and ocularists are superior sulcus deformities from inadequate orbital volume and eyelid ptosis or laxity.
The Ocularist’s Work
Prosthetic eyes are often called “glass eyes” because, before the development of polymethyl-methacrylate plastics in the 1940s, prosthetic eyes and ocular implants were generally made of hand-blown glass, a technique that dates to the mid-1800s. (Cryolite glass is still used in parts of Eastern Europe.)
While careful postsurgery observation by other professional “Os” in eye care is often assumed to provide adequate evaluation of the socket, many irregularities are only discovered when the alginate mold (or “impression”) of the healed socket made in the ocularist’s office is examined. The initial visit to the ocularist usually takes place 6 weeks after surgery. Though most swelling has usually subsided by this time, only after 3 or 4 months is the healed socket’s shape stabilized.
Most ocularists begin by obtaining an alginate (gel) impression of the eye socket, the sensitive tissue which will house the prosthetic eye. (Although this is a painless procedure, some younger patients may find the one-minute setting time uncomfortably long.) Duplicating the socket shape precisely reduces irritation of the conjunctiva and maximizes the movement of the finished eye. When the proper fit is achieved, the lubricating tear system often operates normally. After the impression and fitting of a wax pattern, the resulting shape is cast in plastic.
Next, the ocularist hand-paints the iris and sclera using direct observation of the patient's unaffected eye, mixing a variety of pigments, lacquers, or oils onto the acrylic shape, bonded with liquid acrylic (see figure 2). The painting is sealed with acrylic, and a cornea of clear plastic is cast and cured under heat and pressure. Polishing the eye to a flawless surface ensures there will be smooth eyelid movement and no recesses to accommodate flora.
Figure 2. The Process of Fabricating an Artificial Eye in Acrylic, as Seen in Stages.
Caption
Stage A. The gel impression (negative) of the socket
Stage B. The wax pattern cast from the impression and fitted further
Stage C. An acrylic shape sized to the socket and refined as to gaze
Stage D. The painted prosthesis just out of the mold and before polishing
Stage E. The final prosthesis ready to insert
When the finished eye is inserted, the patient is given a mirror to see his or her restored image (see figure 3). Care of the prosthetic eye is simple; new patients are often surprised to learn that they need not remove it for routine washing—a cleaning and polishing by the ocularist during each annual examination is sufficient.
Figure 3. Left: A Monocular Patient with an Empty Socket. Right: The Patient Wearing a Prosthesis.
Refinements in surgical procedures, ocular implants (including materials) and custom hand painted prosthesis have made great improvements in the cosmesis and comfort of prosthetic eye wearers.
This brief article is merely an introduction to the profession of custom ocularistry—the fourth “O.” More information is available from the American Society of Ocularists and its journal, The Journal of Ophthalmic Prosthetics.