Abstract
The goal of plastic surgeons performing postmastectomy anatomic reconstruction is to create a breast structure that closely matches the shape and appearance of a patient’s native breast. Tattoo artists have helped improve outcomes with nipple-areolar tattooing. Some patients now prefer to have more extensive, nonanatomic designs to help camouflage their scars. Two questions are considered here: What role should plastic surgeons have in supporting or performing nonanatomic reconstruction? And should insurance programs cover nonanatomic breast reconstruction options?
Introduction
For many plastic surgeons, breast reconstruction is the most common procedure in their practices. Over 300,000 women were diagnosed with breast cancer or in-situ disease in 2017, with many of those patients undergoing either partial or total mastectomy [1]. On an annual basis, over 100,000 breast reconstruction procedures are performed by members of the American Society of Plastic Surgeons [2]. Following passage of the Women’s Health and Cancer Rights Act in 1998, all group plan insurers who covered mastectomies were also required to cover postmastectomy breast reconstruction [3]. Multiple large studies have demonstrated the health benefits of postmastectomy breast reconstruction, including physical, psychosocial, and sexual well-being, for women with breast cancer [4].
Fundamentally, the goal in breast reconstruction is to recreate a breast that has a “normal” appearance. The use of “normal” here reflects the wide variation that exists in natural breast shape and size, but it also indicates that the shape and form of a particular woman’s breast would still be reconstructed to be within the bell curve of native breast anatomy. If it is the patient’s wish, it would be ideal to recreate the exact same shape, size, and contours of her breasts that existed prior to cancer treatment. However, the limitations of breast reconstruction techniques makes meeting a standard of normal shape the end goal, even if that shape is not the patient’s exact previous shape. Depending on the specific surgical technique, women can have some choice in the subsequent size and shape of the breast, although this choice is not guaranteed and still must be within the normal range of breast shape and size.
Nipple-Areolar Tattooing
Women interested in postmastectomy breast reconstruction usually have three options—external prosthesis, implant-based reconstruction, or autologous reconstruction via transfer of adipose tissue from another area of their body. Many patients have removal of the nipple-areolar complex as part of the mastectomy and thus nipple reconstruction is often the final stage of reconstruction after completion of the breast mound. This is frequently done by using local tissue to create a papule followed by areolar tattooing to provide the darker pigment seen in the native breast. Most areolar tattooing is done in the plastic surgeon’s office by either the physician or a physician extender. Figure 1 demonstrates a completed bilateral breast reconstruction using transplanted tissue from the patient’s lower abdomen followed by papule reconstruction and areolar tattooing.
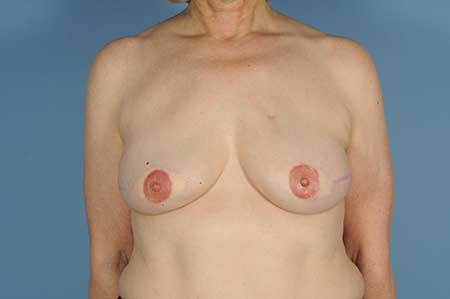
Figure 1. Postmastectomy Breast Reconstruction with Bilateral Autologous Tissue, Nipple Reconstruction, and Areolar Tattooing. Photo: Jeffrey H. Kozlow.
Thankfully, plastic surgeons are not alone in trying to provide the best outcomes for their patients. Within the last ten years, professional tattoo artists in our local communities have played an increasing role in nipple-areolar tattooing, including the use of 3-D tattoos to give the appearance of a papule without the need for a surgical procedure. This movement, led by Vinnie Myers, a tattoo artist in Baltimore, has now been embraced by professional tattoo artists in almost every major city, providing our patients with another option for nipple reconstruction [5]. Traditionally, these tattoo artists have relied on patients seeking out their tattooing services, but increasingly plastic surgeons are referring patients directly. Importantly, nipple-areolar tattoos are done to recreate the appearance of an individualized but anatomically normal nipple-areolar complex, and they do so in an amazing fashion.
Tattooing as an Alternative to Surgical Breast Reconstruction
Not every woman who undergoes surgical treatment for breast cancer is interested in formal breast reconstruction. Some women who undergo mastectomy are not interested in breast reconstruction based on their own personal choices and values. Other women might undergo breast mound reconstruction only and forego nipple areolar reconstruction. There are also women who undergo breast conservation therapy (BCT), a combination of surgical lumpectomy and radiation therapy, instead of mastectomy. This treatment can often lead to both subtle and significant deformities of the treated breast. Regardless, all of these women are left with surgical scars that can be a frequent reminder of their personal battle with breast cancer.
Some women have turned to artistic tattooing to help camouflage their scars while others have decided to go further and turn their chest into an art canvas. The ability of professional tattoo artists to provide another option for our breast cancer patients has been highlighted in both social media and a recent article published in the Journal of the American Medical Association (JAMA) by tattoo artist David Allen [6]. Movements such as P.ink highlight that nonanatomic tattooing can provide some women a therapeutic option that differs from surgical breast reconstruction [7]. And though there is no formal study on patient reported outcomes, I have no reason to doubt that, for the women who seek it out, this type of tattooing has a positive impact on their quality of life, self-confidence, and body image. With regard to nonanatomic tattooing as an option for our patients, I do think it is important that we are aware of this type of work and that for some patients it may be what best suits them. Just as most surgeons discuss an external prosthesis as an option for breast mound reconstruction, I think it is important that we be aware of camouflage tattooing and supportive of those patients who opt for it.
Ethical Issues in Nonanatomic Breast Reconstruction
The topic of breast reconstruction generates two potential ethical questions for plastic surgeons. The first question is whether plastic surgeons should perform procedures aimed at producing results that are not congruent with the typical appearance of a normal breast. Fundamentally, the goal of any reconstructive procedure is to recreate as close to normal anatomy and function as possible regardless of the site or etiology of the defect. While there may be fringe examples of surgeons who will perform nonanatomic reconstructive surgical procedures that produce results well outside the range of normal anatomy, these would be rare individual surgeons. Despite what can be seen on television, the vast majority of board-certified plastic surgeons will not perform procedures that create abnormal anatomy even under the guise of “cosmetic surgery.” I personally believe that almost all board-certified plastic and reconstructive surgeons would find it unethical to create abnormal anatomy unless for specific functional reasons. This fundamental principle is a critical component of what makes our work medically necessary and is integral to the care of many patients. We all occasionally get atypical patient requests regarding their goals for breast reconstruction. Some of these requests, such as placing multiple implants in the same breast or inflating implants beyond manufacturing limits, are not surgically safe [8]. Others, such as requests for breast reconstruction in areas outside of the anterior chest or axillary nipple position or for the use of nonanatomic shaped implants, can raise concerns about unrealistic patient expectations for breast reconstruction or potential mental health problems. I can understand how patients who make a minor request—for example, for a heart-shaped areola instead of a circular areola—might find this a subtle therapeutic or “fun” way to deal with their breast cancer diagnosis. Accepting these women’s request as a unique way to deal with their breast cancer diagnosis and accepting the rationale behind their request seem logical.
However, I personally still decline to perform any form of nonanatomic breast reconstruction procedures, as I believe that doing something slightly different becomes a slippery slope to creating abnormal anatomy. Thus, for professional consistency, I believe that reconstructive surgeons should only be performing breast reconstruction procedures aimed at restoring either the patient’s premastectomy anatomy or, in cases where this is not technically possible, anatomy that would otherwise be consistent with normal breast anatomy in terms of size, shape, and nipple-areolar appearance. Reconstructive surgeons can also refer patients to individuals or services that provide alternatives to surgical breast reconstruction such as camouflage tattooing. However, failure to inform a patient of these alternative options does not constitute a breach in duty given that camouflage tattooing is not considered a current standard of care.
The second, similar question is whether insurance plans should cover alternatives to reconstruction of the typical appearance of a normal breast, including nonanatomic tattoos. Some insurance plans will cover professional, anatomic nipple-areolar tattooing performed outside of a physician’s office, although it depends on the insurer and the explanation of benefits. In my experience, many women have found securing insurance coverage for anatomic nipple-areolar tattooing outside of a physician’s office to be a challenging endeavor. I believe that the same ethical requirement on physicians to perform only anatomic reconstructions should apply to insurers’ considerations of which procedures to cover and why. It is important to recognize that breast reconstruction patients are not the only patients who might choose to get a nonanatomic tattoo. People might get a tattoo for therapeutic reasons, including remembrance of a death, celebration of overcoming an obstacle in life, or camouflaging of a traumatic injury. Despite the benefits, many people might not expect insurance coverage of the tattooing procedure for any of these valid therapeutic reasons since it is not intended to restore normal anatomy. The view for which I argue here—that nonanatomic tattooing should not be covered by insurance—seems consistent with those expectations.
Plastic and reconstructive surgeons frequently have to decide when requests for surgery are for functional versus aesthetic indications. Admittedly, the line between the two is not always clear and opinions rightly vary. For example, when is a congenital breast asymmetry significant enough to be considered reconstructive rather than aesthetic? When is a scar unfavorable enough to warrant scar revision? Or when is extra abdominal skin following weight loss a functional impairment? For each surgical request, the decision is made from a professional standpoint and, when applicable, should conform to what insurers prescribe within the explanation of benefits to a patient. Performing surgery for aesthetic reasons is still ethical, but it is important to be clear about the aesthetic indication and, if expecting reimbursement from insurance, to ensure that it meets the necessary requirements of a given plan.
Conclusion
I applaud the work of the tattoo artists who are helping women in their personal journeys through breast cancer treatment and recovery. Whether it is a 3-D nipple-areolar tattoo or more extensive tattooing to hide the scars from breast cancer, I believe that the work is good and that patients are benefitting from the procedures. I believe that our patients have the autonomy to choose to undergo those interventions that they believe will be most beneficial to them. However, we professions must also retain consistency in our goals of reconstruction to restore normal anatomic structures or function, especially when the responsibility for payment is a public or private insurance plan.
References
-
American Cancer Society. Breast cancer facts and figures 2017-2018. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/breast-cancer-facts-and-figures/breast-cancer-facts-and-figures-2017-2018.pdf. Published 2017. Accessed January 2, 2018.
-
American Society of Plastic Surgeons. 2016 Plastic surgery statistics report. https://www.plasticsurgery.org/documents/News/Statistics/2016/plastic-surgery-statistics-full-report-2016.pdf. Accessed January 2, 2018.
-
Centers for Medicare and Medicaid Services. Women’s Health Care Rights Act (WHCRA). https://www.cms.gov/CCIIO/Programs-and-Initiatives/Other-Insurance-Protections/whcra_factsheet.html. Accessed February 2, 2018.
- Platt J, Zhong T. Patient-centered breast reconstruction based on health-related quality-of-life evidence. Clin Plast Surg. 2018;45(1):137-143.
- Allen D. Moving the needle on recovery from breast cancer: the healing role of postmastectomy tattoos. JAMA. 2017;317(7):672-674.
- Halvorson EG, Cormican M, West ME, Myers V. Three-dimensional nipple-areola tattooing: a new technique with superior results. Plast Reconstr Surg. 2014;133(5):1073-1075.
-
P.ink website. http://p-ink.org/. Accessed January 19, 2018.
-
Mentor®. Saline-filled and SPECTRUMTM breast implants. http://www.mentorwwllc.com/Documents/SalineSpectrumPIDS.pdf. Revised May 2015. Accessed January 19, 2018.



